Project Description
A summary of articles and research around accuracy and limitations of CT-Based Guided Surgery.
Journal of Prosthetic Dentistry – 2009
Problem: “Limited surgical access with surgical guides intraorally may be one of the most common challenges of using surgical guides. Surgical guides may interfere with effective use of surgical instruments in the posterior segments where interocclusal distance may be limited, especially for the partially edentulous patient.”
Solution: “Surgical guides for implant placement should be designed not only as a precise and effective communication tool, but also to occupy minimum space so as not to interfere with the surgery.”
Park et al, Accuracy of Implant Placement Using Precision Surgical Guides with Varying Occlusogingival Heights: An in Vitro Study. JOPD 2009;101.6:372-381
International Journal of Oral & Maxillofacial Implants – 2011
“The incorporation of treatment planning modified by CAD/CAM offers significant advantages, including the evaluation of three-dimensional anatomy and the fabrication of anatomic site models and bone-supported surgical templates. Other advantages are shorter treatment times, minimization of intraoperative radiography during implant placement, less invasive surgical techniques (eg, flapless surgery with less swelling and pain and faster initial healing times), prefabrication of a definitive prosthesis, and immediate use of a fixed prosthesis. (5,17)”
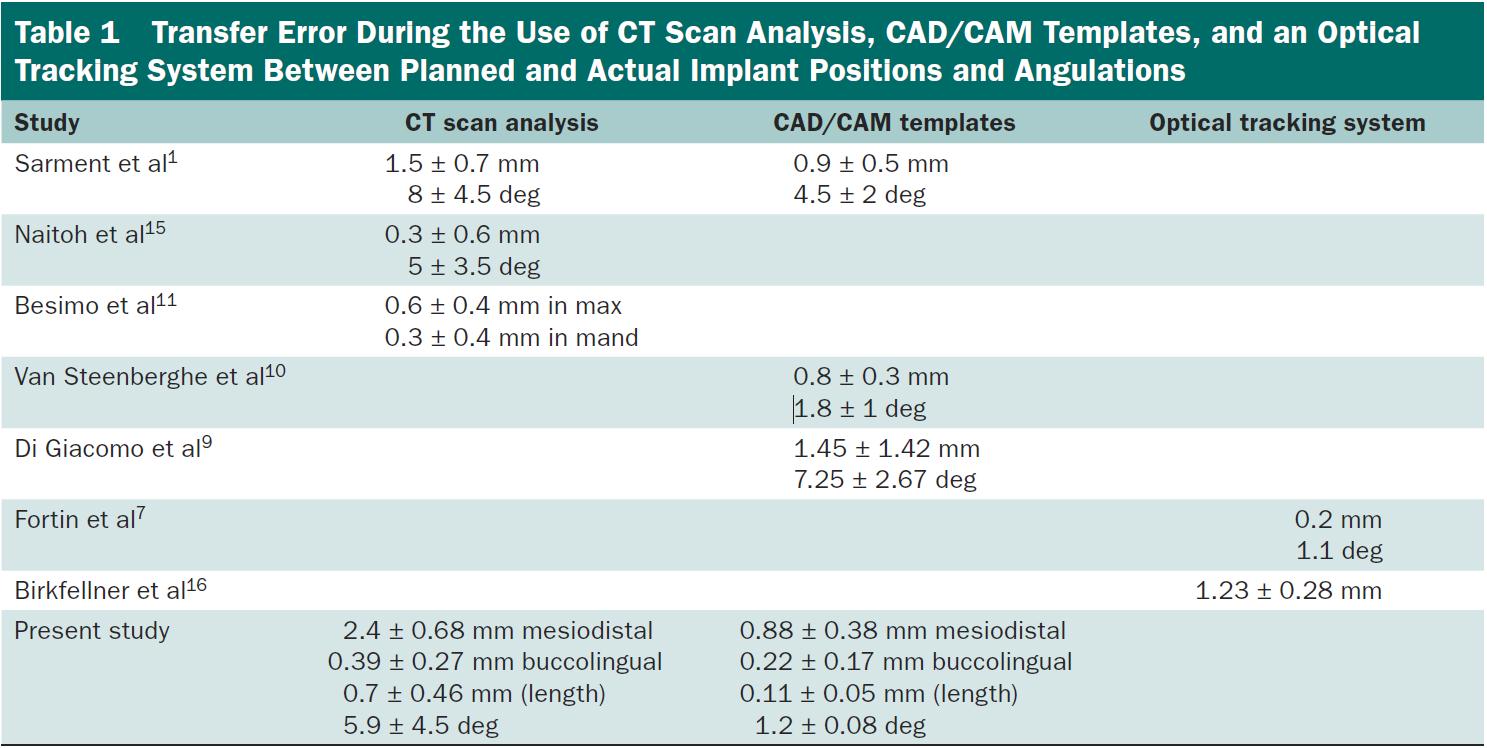
“Based on the results of the present study, it was noted that the differences between planned and actual implant positions and angulations with the CAD/CAM method were smaller than those placed using a conventional planning method. Table 1 summarizes the results obtained in this study and compares them to previous studies.”
“The average differences between the planned and actual entry points in the mesiodistal and buccolingual directions, lengths, and angles of the implants and the osteotomy showed a considerable reduction in the CAD/CAM group versus the conventional group (P<.005).”
Nokar et al, Accuracy of Implant Placement Using a CAD/CAM Surgical Guide: An In Vitro Study. IJOMI 2011;26:520-526
International Journal of Oral & Maxillofacial Implants – 2013
“Clinical evidence has shown that CAD/CAM surgical guides are accurate, and two in vitro studies showed that they were more reliable than conventional guides in reproducing planned implant positions… This study therefore sought to compare the accuracy of CBCT-guided CAD/CAM surgical guides with that of conventional guides in the same patient population.”
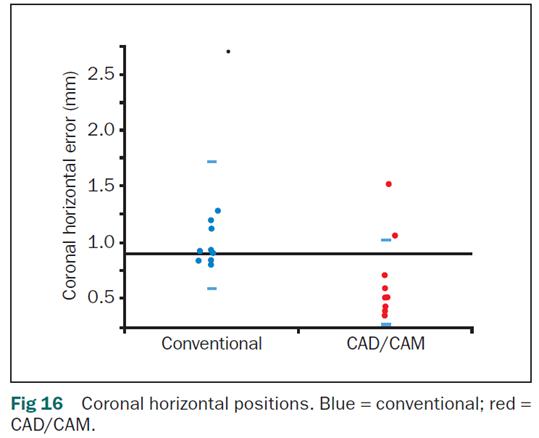
Results: “Implants placed with CAD/CAM guides were closer to the planned positions in all eight categories examined. However, statistically significant differences were shown only for coronal horizontal distances. It was also shown that CAD/CAM guides had less variability than conventional guides, which was statistically significant for apical distance.”
Conclusion: “Implants placed using CAD/CAM surgical guides provided greater accuracy in a lateral direction than conventional guides. In addition, CAD/CAM guides were more consistent in their deviation from the planned locations than conventional guides.”
“Within the limitations of this prospective clinical study, the following conclusions were made.”
“1. Single implants placed with computer-generated surgical guides were generally closer to the planned positions than those placed with conventional guides.
2. Differences in the accuracy of these guide types were statistically significant for coronal horizontal distances (P=.0409).”
Farley et al, Split-Mouth Comparison of the Accuracy of Computer-Generated and Conventional Surgical Guides. IJOMI 2013;28.2:563-572
Journal of California Dental Association – 2008
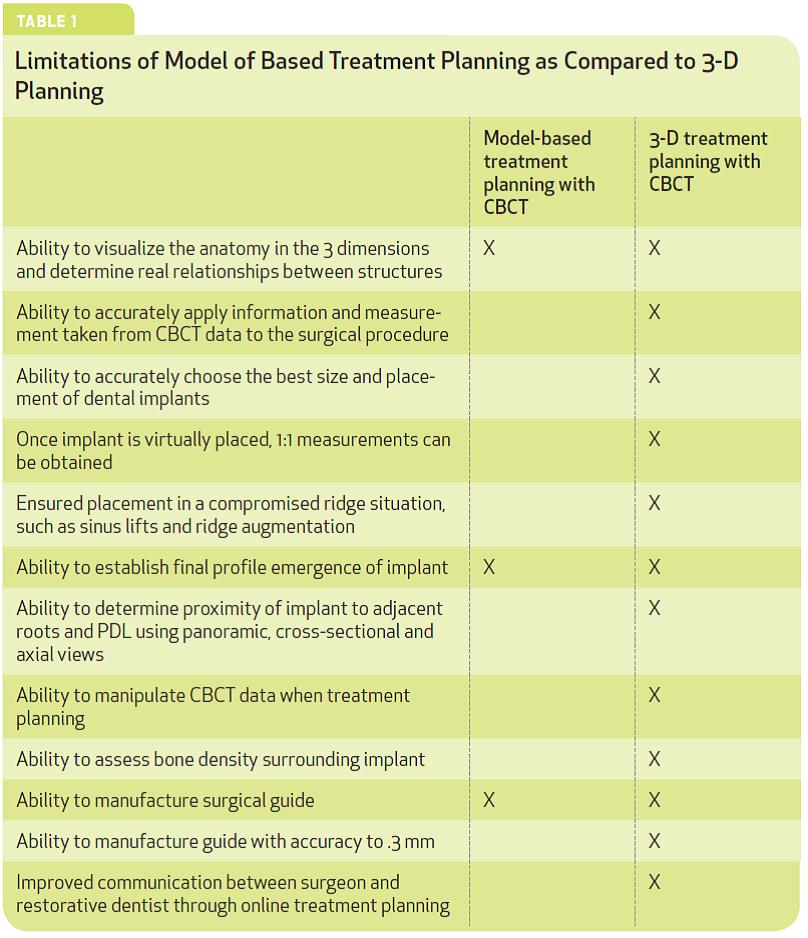
“CBCT and 3-D treatment planning are emerging technologies for dentistry that offer alternative imaging options between 2-D imaging and model-based planning… CBCT and 3-D imaging also improve the communication between the surgeon, restorative dentist and patient. Through the 3-D treatment planning the clinician is better able to understand the limitations that may be encountered in surgery before a flap is laid. These imaging and manufacturing capabilities do not exist with 2-D imaging and model-based treatment planning (Table 1).”
“CBCT and 3-D treatment planning are emerging technologies that provide the clinician with the necessary information for routine and complex cases involving the placement of implants in the mandible or maxilla.”
Peck J, Radiologic Techniques Using CBCT and 3-D Treatment Planning for Implant Placement. JCDA 2008:36.4:287-297
Journal of Oral & Maxillofacial Research – 2012
Clinical Considerations in Selection Criteria for Dental Implantology: “Over the past decade, there has been a dramatic conceptual shift from a surgically driven to a prosthetically driven approach to dental-implant therapy.(5,14,17,26,27) It is no longer acceptable practice to place implants in alveolar bone without a previously developed plan for prosthetic restoration. To optimize implant placement and to avoid surgical complications, the clinician must have full knowledge of oral-bone anatomy so that any osseous-topography, bone-volume excesses/deficiencies can be corrected before implant placement.(28-31)”
Rotational panoramic radiography: “Because of its inherent limitations, panoramic radiography is considered unsuitable as a single imaging source for dental-implant site assessment.(7,11-13,51,56-58)”
Cross-sectional imaging techniques: “Cross-sectional imaging techniques produce in-focus, thin-section images… The main advantage of these images for implant dentistry is that they minimize or eliminate anatomic superimposition. Image sections perpendicular to the long axis of the region (object) of interest (e.g., the mandibular arch) are referred to as crosssectional trans-axial images. Cross-sectional images provide optimal accuracy for visualizing the bony architecture of the jaws.”
Recommendation 4. “The radiographic examination of any potential implant site should include crosssectional imaging orthogonal to the site of interest.”
Recommendation 5.”CBCT should be considered as the imaging modality of choice for preoperative crosssectional imaging of potential implant sites… The use of CBCT before bone grafting helps define both the donor and recipient sites, allows for improved planning for surgical procedures, and reduces patient morbidities. CBCT is best for the evaluation of volumetric and topographic changes of the restored residual alveolar ridge.”
Recommendation 7. “CBCT imaging should be considered if bone reconstruction and augmentation procedures (e.g., ridge preservation or bone grafting) have been performed to treat bone volume deficiencies before implant placement.”
Conclusions: “Initial imaging assessment is best achieved with panoramic radiography and may be supplemented with periapical radiography. For the preoperative diagnostic phase, the AAOMR reaffirms that cross-sectional imaging be used for implant site assessment. Furthermore, the AAOMR recommends CBCT imaging as the current method of choice for cross-sectional imaging in that it provides the greatest diagnostic yield at an acceptable radiation dose risk. The decision to perform a CBCT examination must be clinically justified and based on professional judgment (that is, the judgment of the clinician is that the use of CBCT will potentially provide information needed for prosthetic treatment planning, implant selection, and/or surgical placement). The CBCT imaging protocol should include the smallest FOV necessary and available and optimize exposure parameters. For periodic, postoperative implant monitoring, periapical and, in some cases, panoramic images provide adequate imaging.”
Tyndall et al, Position Statement of the American Academy of Oral and Maxillofacial Radiology on Selection Criteria for the Use of Radiology in Dental Implantology with Emphasis on Cone Beam Computed Tomography. JOMR 2012;113.6:817-826
Journal of California Dental Association – 2003
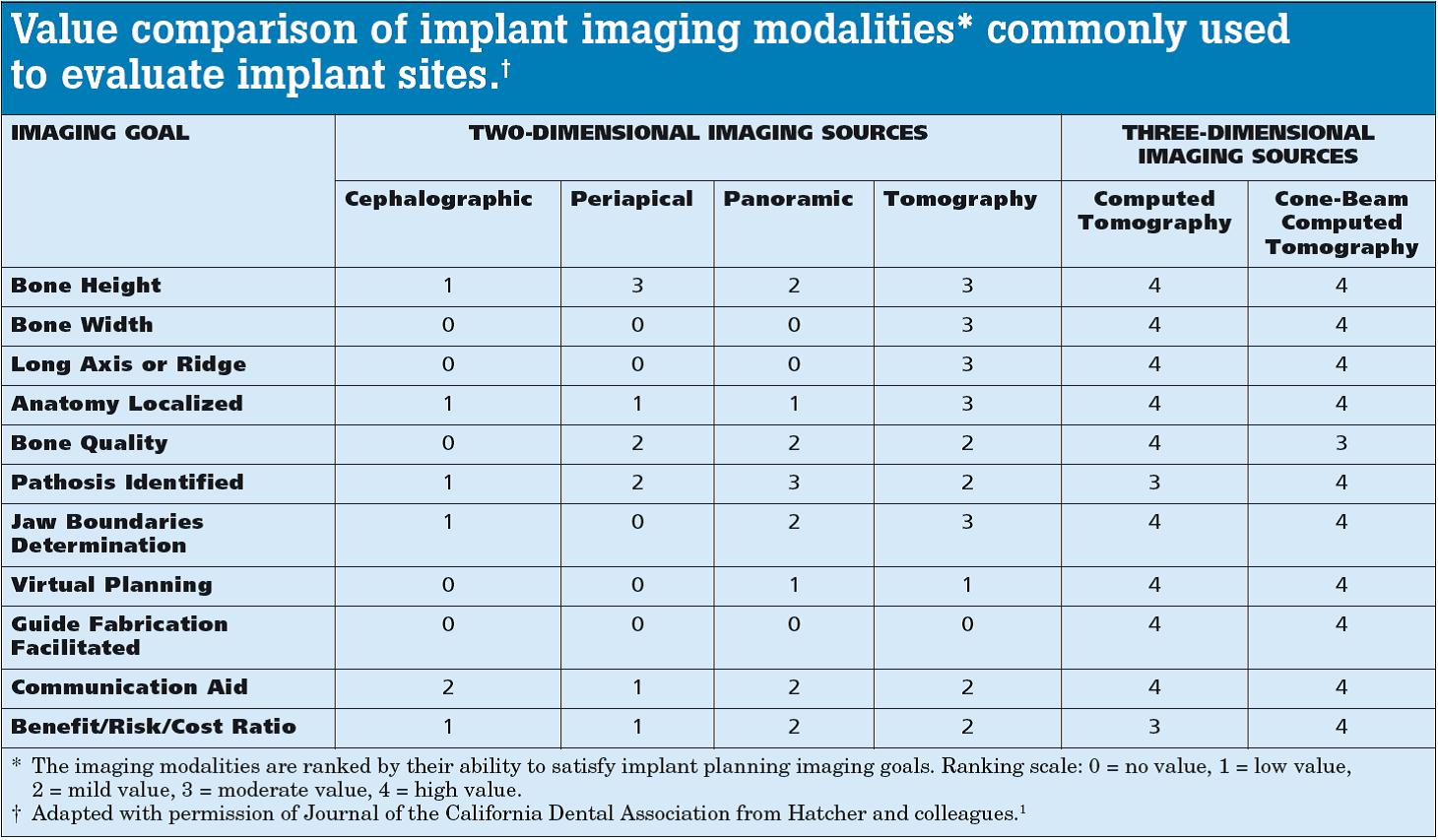
“Diagnostic information, treatment planning and treatment benefits levels have increased with the use of 3-D imaging techniques. Using 3-D virtual planning techniques before treatment has resulted in optimal implant placement and improved clinical outcomes. The development of 3-D scanning such as cone-beam computed tomography (CBCT) instead of planar films has led to improved visualization and comprehension of the anatomy in the areas in which implants are being planned for placement. Computed tomographic (CT) scans and CBCT scans reproduce the anatomy with a submillimetric accuracy.”
Hatcher DC, Dial C, Mayorga C. Cone Beam CT for Pre-Surgical Assessment of Implant Sites. JCDA 2003;31(11):825-833
Journal of the American Dental Association – 2010
“CBCT provides the anatomical data that can generate a collaborative treatment plan and achieve optimal outcomes for the restorative dentist, radiologist, surgeon and patient. The evolution in CBCT hardware and software has been responsible, in part, for the increase in the precise planning and placement of implants while minimizing the associated risks.”
Worthington P, Rubenstein J, Hatcher D, The Role of Cone-Beam Computed Tomography in the Planning and Placement of Implants. JADA 2010;24.141:19S-24S
International Journal of Oral & Maxillofacial Implants – 2010
“The use of computerized tomography (CT) has become mainstream in aiding the diagnosis of available bone volume and quality at potential implant sites as well as location of related anatomical structures including, but not limited to, the maxillary sinuses, inferior alveolar nerve, and teeth. The use of medical CT remains a principle source for most clinicians but the advent of cone beam computed tomography (CBCT) scan imaging techniques are rapidly increasing in popularity, not least due to the significantly lower effective dose of radiation, consistent with principles of good radiation practice. To this end, it has been proposed that CBCT now fulfills the requirements to be considered a standard of care in the diagnosis and planning ofimplanttreatment. (18)”
2010 Guidelines for the Provision of Dental Implants and Associated Patient Care Task Force, 2010 Guidelines of the Academy of Osseointegration for the Provision of Dental Implants and Associated Patient Care. IJOMI 2010;25.3;620-627

Comments are closed.